OGX-110 is a small-molecule drug candidate that selectively activates the CXCR3 pathway, the pathway most strongly implicated in pruning neovascularization, limiting fibrosis, and restoring homeostasis in wound healing.
While existing treatments for these three targeted diseases block a single growth factor that drives vascular proliferation (generally VEGF), OGX-110 targets a pathway that overrides the numerous factors that drive angiogenesis and fibrosis. By activating CXCR3, OGX-110 induces the regression of abnormal blood vessels and fibrotic tissue, preserving the pre-existing vascular and fibrotic infrastructure and thereby restoring homeostasis.
The Wound Healing Paradigm
Like every biological process in the human body, wound healing occurs through specific and highly coordinated phases: hemostasis/inflammation, tissue replacement, and resolution. For a wound to heal properly, all phases must happen in the correct order and within the right time frame. During this final phase, wound resolution, all the cell and matrix resources recruited during tissue replacement diminish, returning the system to homeostasis. In this phase, over 90% of the vasculature and two-thirds of the matrix regress as the tissue regenerates.
Specific signals initiate this resolution phase by activating a cell surface receptor, CXCR3, which is the most important. Activation of this pathway is triggered by naturally occurring chemokines, with IP-10 being the main one. This signaling axis, IP-10, and CXCR3 are acute-phase molecules that are significantly upregulated to end the tissue replacement phase of wound healing and begin resolution. Failure to properly activate this axis leads to chronic inflammation, fibrosis, and permanent scarring. This occurs when the wound bed fails to sense completion through contact inhibition and remains in the tissue replacement phase. By pharmacologically activating the CXCR3 signaling pathway, it is possible to restore chronic wound processes to a state of homeostasis.
The Four Mechanisms of OGX110
Angioregression
Pathological neovascular membranes regress as CXCR3 activation causes endothelial cell anoikis. Clinical evidence: CNV area reduced from 6.5 to 1.7 mm² in representative patient over 6 months, continuing after drug clearance.
Anti-Inflammatory
Recruitment of M2-suppressor macrophages and regulatory T-cells reduces intraretinal inflammation independently of fluid reduction. Manifests as improved BCVA beyond anatomical changes alone.
Anti-Fibrotic / Anti-Scarring
OGX110 suppresses development of subretinal fibrosis — the leading cause of irreversible vision loss in AMD. Clinical evidence: >80% SHRM resolution vs. 28–30% for anti-VEGF agents. Only therapy in the clinic with this claim.
Restoration of Homeostasis
CXCR3 signaling recruits and supports tissue stem cells, helping maintain vision-critical photoreceptors. Clinically manifests as extended treatment-free intervals (6+ months) with stable or improving BCVA.
Our Target Indications
Wet Macular Degeneration
About 200,000 new cases of wet AMD are diagnosed each year in North America. Due to the aging population, the National Eye Institute estimates that the prevalence of advanced AMD will grow to 5 million by 2040.
In wet AMD, an aberrant wound response leads to the proliferation of blood vessels and a fibrotic growth starting in the macula, the area of the retina responsible for central vision. Damage to photoreceptors in the macula can cause distortion or blind spots in a person’s central vision. Patients with wet AMD who are untreated or for whom treatment is ineffective (about 30% to 50%) can progress to total blindness. VEGF inhibitors address the edema released by this pathological vasculature in most patients, with most of these becoming less responsive over time; thus, there is a need for other mechanisms to reduce the edema. More importantly, the anti-VEGF therapies do nothing to cause the regression of the pathological vessels or limit the fibrosis responsible for the long-term loss of sight. This is an unmet clinical need not addressed by any other compounds in development for AMD.
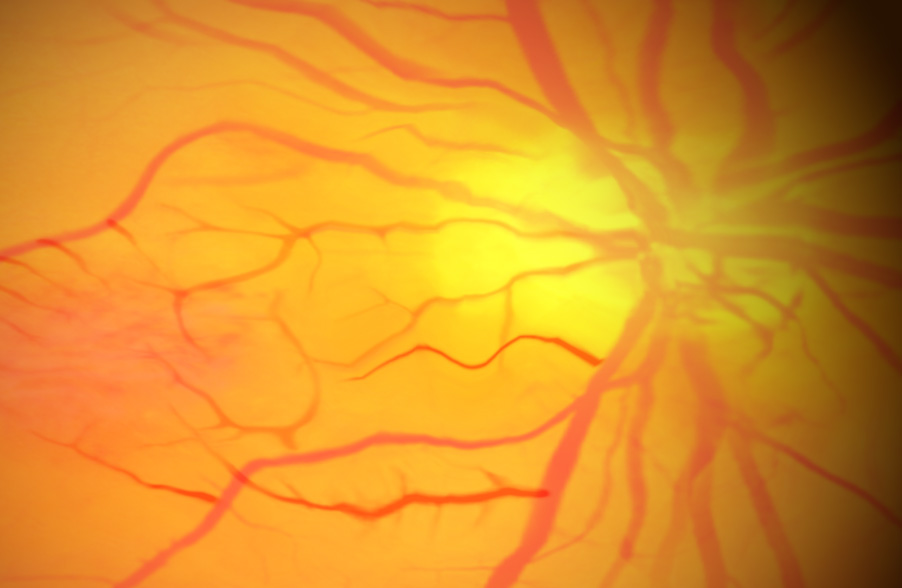
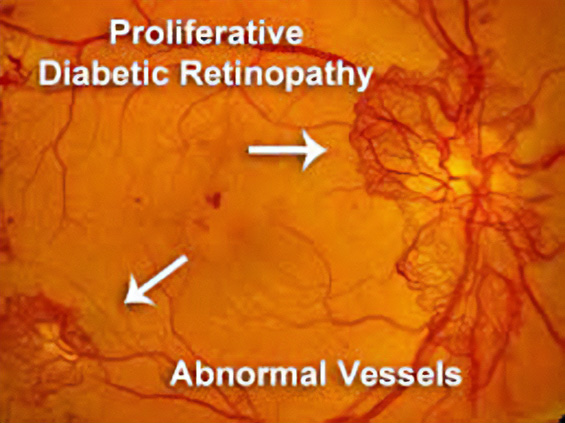
In 2021, across all ages, an estimated 9.6 million people in the United States were living with diabetic retinopathy (DR). Of these, 1.84 million were living with vision-threatening proliferative DR (pDR) or late-stage Diabetic Retinopathy. In diabetic retinopathy, abnormal, “leaky” blood vessels release fluid and can cause hemorrhages. At the advanced stage of the disease, new vessels infiltrate the retina, leading to the formation of fibrotic tissue on the retinal surface or in the vitreous cavity, vitreous hemorrhage, retinal detachment, retinal damage, and loss of vision.
These blood vessels, which are thin, weak, and prone to bleeding, cause scar tissue to form inside the eye. This scar tissue can pull the retina away from the back of your eye, causing retinal detachment. A detached retina typically results in blurriness, a reduced field of vision, and, in severe cases, permanent loss of vision. Laser photocoagulation is often effective; however, the procedure can be painful and may result in loss of peripheral vision. Anti-VEGF therapies are effective for a large percentage of patients, but as many as 25% do not respond even at the start, and many more become resistant over time.
OGX-110 has been shown to cause the regression of these nascent pathologic vessels in the animal model of pDR and to suppress the development of fibrosis. This novel mechanism of action holds great promise for improving sight in the short term and ultimately shutting down the drivers of the disease.
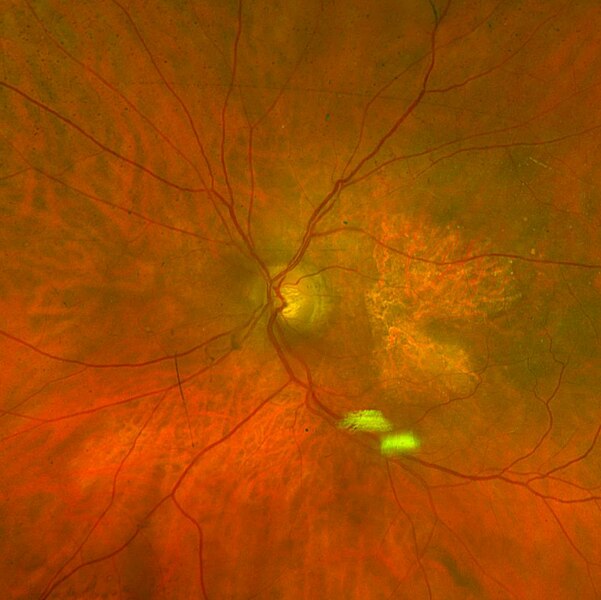
Geographic Atrophy
More than 5 million people worldwide have geographic atrophy, including nearly 1 million in the U.S. In developed nations, approximately 1 in 29 people over the age of 75 have geographic atrophy, which increases to almost 1 in 4 people over the age of 90.
With aging, the retinal pigment epithelium (RPE) is exposed to intrinsic and extrinsic oxidative and environmental stressors such as cigarette smoke. The cytotoxic damage accumulates, resulting in the formation of drusen, yellow deposits of lipids between the RPE and Bruch’s membrane. Excessive drusen accumulation and drusen components, such as cellular debris, lipids, and lipoproteins, may trigger chronic inflammation through multiple pathways, including a chronic wound response. Chronic inflammation, a result of the wound response, can eventually lead to photoreceptor, RPE, and choriocapillaris cell death, causing the appearance of sharply defined atrophic lesions that are characteristic of GA and the appearance of choroidal vessels due to the missing RPE layer.
Two therapies limiting different aspects of the complement cascade were recently approved as the first agents to treat GA. Unfortunately, each of these agents reduces the growth rate of the lesions by only about one-quarter and, therefore, does not significantly impact the retention of visual acuity, at least within the first year or two. This continued progression of the disease demonstrates a gap in treatments and argues for new mechanisms by which to shut down the chronic wound response that leads to GA.
By activating the CXCR3 pathway, OGX-110 triggers an irreversible molecular cascade that resolves the wound response, suppressing inflammation, the development of fibrosis, and the regression of the choroidal vessels.
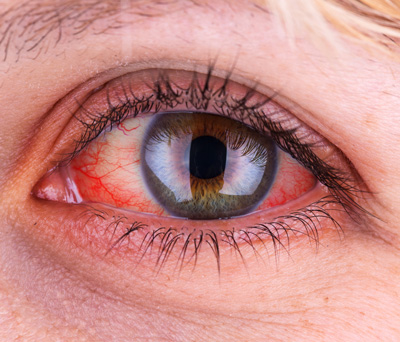
Dry Eye
Approximately 39 million patients in the United States suffer from Dry Eye Disease (DED). Symptoms include ocular pain, dryness, and a persistent, gritty sensation, which are all too familiar persistent aspects of the disease. DED can be secondary to many insults, the major ones being dry or salty air, air pollution, surgical damage of the ocular surface, and viral and autoimmune diseases. The commonality of all these causes is that a loss of tears eventually damages the goblet cells that produce the mucin that binds the tears to the eye’s surface.
There are presently five FDA-approved therapeutics for the treatment of dry eye disease. The first one, Restasis, was approved twenty years ago, but the pace of approvals has picked up significantly in the last three years. While most approved therapies focus on limiting the autoimmune activation that can lead to DED, the vast majority of DED is caused by environmental, chemical, and surgical insults. This singular focus on immune-driven DED is one of the main reasons that existing drugs have such marginal benefits.
Significant unmet clinical needs remain. The largest of these are treatments that can impact the goblet cells, the origin of mucin, and meibomian gland dysfunction (MGD), the source of the lipid layer in tears. Our animal studies demonstrate that our therapy, which causes the regeneration of goblet cells, can positively affect environmental, surgical, and chemical-based DED. As the goblet cell functioning is central to DED, and we have found that our agent can restore this function, Ocugenix is uniquely positioned to be disease-modifying in DED.
Mechanism of Action
OGX-110 selectively activates the CXCR3 pathway via the physiologic binding site. The CXCR3 pathway has been well-characterized in wound healing, regulating both fibrosis and angiogenesis. This pathway restores wound healing toward a regenerative state by noncompetitively overriding pro-angiogenic and pro-fibrotic signals from various growth factors, including VEGF.
In retinal diseases, activating this same pathway is expected to produce an anti-fibrotic and angio-regressive effect that would not only arrest disease progression but potentially reverse it. Ocu-110 is derived from a naturally occurring activator of the CXCR3 pathway, which has been vetted in preclinical and clinical studies, demonstrating its ability to regress vascularization and inhibit fibrosis. As it is a physiologic activator of CXCR3, there has been no evidence of toxicity in any of our preclinical studies.
Advantages of a New Mechanism of Action
Current therapies for the target indications are either incomplete or suboptimal. In most retinal situations, treatments consist of a single mechanism of action, unlike treatments in other indications. Treating patients with therapies that have a variety of mechanisms of action has led to significant advances in nearly all diseases, including oncology and immunology.
Patients with angio-fibrotic retinal diseases such as wet AMD and proliferative diabetic retinopathy, which are driven by a variety of growth factors, would likely benefit from alternative therapeutic approaches in addition to anti-VEGF therapies. The current anti-VEGF therapies address the edema in most patients but do nothing to halt the progression to fibrosis. Additionally, up to one-third of patients do not regain visual acuity with these therapies, and most patients will lose acuity over time, even if they initially respond. Thus, anti-fibrotic treatments and novel approaches to managing edema are needed.
In the chronic fibrotic and scarring condition of GA, the current therapies block a key driver pathway, the complement cascade. However, this only slows progression by about 25%. Other drivers and processes are clearly at work. As CXCR3 signaling overrides chronic fibrosis and restores homeostasis, Ocu-110 should act independently of the complement cascade and provide a new approach to stopping the progression of GA.
- 22-amino-acid peptide mimic of IP-10/CXCL10 (the endogenous CXCR3 activator)
- High selectivity for CXCR3 — equivalent to naturally occurring chemokines, no off-target binding
- Stable ≥3 years as lyophilized product; ≥2 years in aqueous formulation
- New Chemical Entity (NCE) designation — regulatory and exclusivity protections through 2043
- Composition of Matter and Method of Action patents issued worldwide
- Short intraocular half-life (~1.5 days) confirms that observed clinical durability is disease-modification, not pharmacokinetics




